Food & Drug Allergy
ALLERGY & IMMUNOLOGY
GERD Specialist Los Angeles
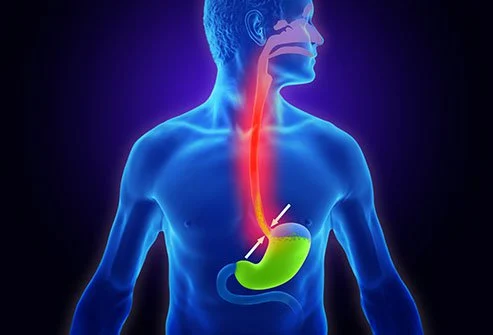
Gastroesophageal Reflux Disease (GERD) is a digestive disorder that occurs when acidic stomach content backs up from the stomach into the esophagus. GERD affects people of all ages—from infants to older adults.
People with asthma are at higher risk of developing GERD. Asthma flare-ups can cause the lower esophageal sphincter to relax, allowing stomach contents to flow back, or reflux, into the esophagus. Some asthma medications (theophylline) may worsen reflux symptoms.
On the other hand, acid reflux can make asthma symptoms worse by irritating the airways and lungs. This, in turn, can lead to progressively more serious asthma. Also, this irritation can trigger allergic reactions and make the airways more sensitive to environmental conditions such as smoke or cold air.
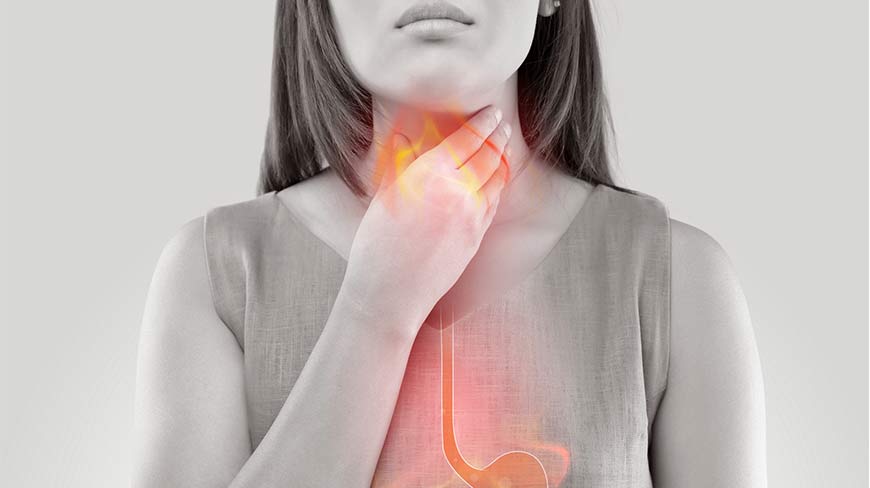
Symptoms
Everyone has experienced gastroesophageal reflux. It happens when you burp, have an acid taste in your mouth, or have heartburn. However, if these symptoms interfere with your daily life it is time to see your physician.
Other symptoms that occur less frequently but can indicate that you could have GERD are:
- Acid regurgitation (re-tasting your food after eating)
- Difficulty or pain when swallowing
- Sudden excess of saliva
- Chronic sore throat
- Laryngitis or hoarseness
- Inflammation of the gums
- Cavities
- Bad breath
- Chest pain (seek immediate medical help)
Diagnosis
Several tests may be used to diagnose GERD including:
- X-ray of the upper digestive system
- Endoscopy (examines the inside of the esophagus)
- Ambulatory acid (pH) test (monitors the amount of acid in the esophagus)
- Esophageal impedance test (measures the movement of substances in the esophagus)
Treatment
If you have both GERD and asthma, managing your GERD will help control your asthma symptoms.
Studies have shown that people with asthma and GERD saw a decrease in asthma symptoms (and asthma medication use) after treating their reflux disease.
Lifestyle changes to treat GERD include:
- Elevate the head of the bed 6-8 inches
- Lose weight
- Stop smoking
- Decrease alcohol intake
- Limit meal size and avoid heavy evening meals
- Do not lie down within two to three hours of eating
- Decrease caffeine intake
- Avoid theophylline (if possible)
Your physician may also recommend medications to treat reflux or relieve symptoms. Over-the-counter antacids and H2 blockers may help decrease the effects of stomach acid. Proton pump inhibitors block acid production and also may be effective.
In severe and medication intolerant cases, surgery may be recommended.
Gerd Specialist Doctor in Los Angeles
Are you suffering from frequent heartburn, regurgitation, or chest pain? You might be experiencing symptoms of Gastroesophageal Reflux Disease (GERD). Finding a specialist who understands your condition is crucial for effective management. Look no further than Dr. Asif Rafi, MD, your trusted GERD specialist in Los Angeles. Dr. Asif Rafi, MD, is dedicated to providing comprehensive care for patients dealing with GERD. With extensive experience and expertise in gastroenterology, Dr. Rafi offers personalized treatment plans tailored to your unique needs. Whether you’re seeking relief from persistent heartburn or seeking solutions for more severe GERD symptoms, Dr. Rafi is here to help.
As a leading GERD doctor in Los Angeles, Dr. Rafi employs advanced diagnostic techniques to accurately assess your condition. From upper endoscopies to pH monitoring, Dr. Rafi ensures thorough evaluation to determine the best course of action for managing your GERD symptoms effectively. What sets Dr. Asif Rafi apart is his commitment to patient education and empowerment. He takes the time to explain your diagnosis, treatment options, and lifestyle modifications in clear, understandable terms. By actively involving you in your care plan, Dr. Rafi empowers you to take control of your health and make informed decisions about managing your GERD.
Whether you require medication management, dietary adjustments, or minimally invasive procedures, Dr. Rafi offers comprehensive solutions to alleviate your GERD symptoms and improve your quality of life. Don’t let GERD symptoms control your life. Schedule a consultation with Dr. Asif Rafi, MD, your trusted GERD specialist in Los Angeles, and take the first step towards relief and recovery. Say goodbye to heartburn and hello to a healthier, happier you with Dr. Rafi by your side.
